State’s trajectory could be lower due to less smokers and early social distancing
Gov. Charlie Baker announced good and bad news on Thursday requiring the anticipated surge of COVID-19 cases in the coming 20 days – with the good news being there are ample Acute beds and the state’s death rate from COVID-19 is lower than other states, and the bad news being that even with an expansion of ICU beds at existing hospitals the state will likely be short up to 500 beds.
State officials, in response, are looking to build Field Hospitals to take the stress off of medical centers – including hiring a contractor that can quickly begin to build out places like the South Boston Convention Center if need be. The plan to build up to 1,000 beds in this fashion around the state.
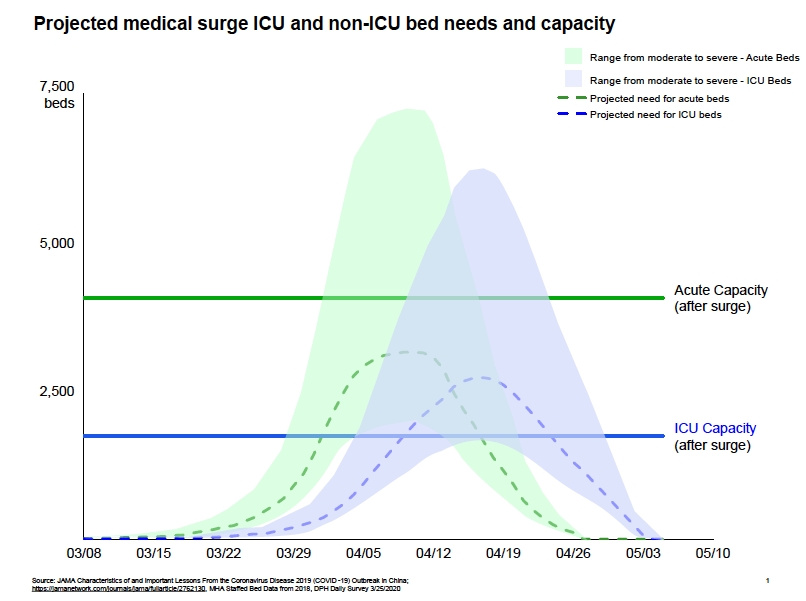
Gov. Baker’s COVID-19 Response Command Center today (April 2) outlined projections related to the anticipated surge of COVID-19 cases in the Commonwealth, which they believe will come between April 10-20.
The projections are the result of the Command Center’s work with medical experts to complete modeling of the outbreak in Massachusetts. The Administration also detailed its efforts to respond to this surge, including a significant increase in hospital capacity, staffing, and equipment.
COVID-19 Surge Planning:
•Modeling and Projections:
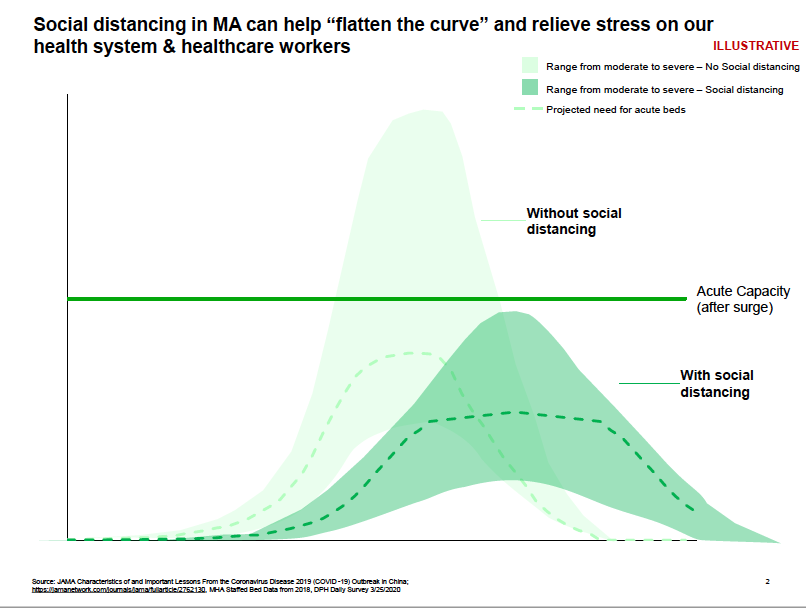
The Administration’s COVID-19 Response Command Center has been working with its Advisory Board of medical experts and epidemiologists from Harvard University, University of Guelph and Northeastern University to refine models related to the expected surge of COVID-19 cases. These efforts include modeling the surge’s timing, number of cases, necessary bed capacity, and work to find facilities that will meet overfill capacity. The model’s projections are based on the experience of Wuhan, China, but Massachusetts’ trajectory could differ due to lower population density, lower smoking rates, and earlier social distancing measures. The Command Center has also been comparing to experience in other states and around the world.
The model’s latest projections estimate that the number of confirmed cases of COVID-19 in Massachusetts could range from 47,000 to 172,000 (or 0.7% to 2.5% of the total population of Massachusetts). The models show hospitalizations would potentially peak between April 10-20. The current fatality rate in Massachusetts is lower than other areas – it is approximately 1.5 percent of those infected. The Command Center is monitoring this statistic closely.
The COVID-19 Response Command Center is working with hospitals to provide them with flexibility to expand ICU capacity. The Commonwealth is asking academic medical centers and teaching hospitals to work to significantly expand their ICU capacity. But after hospitals execute on their surge plans, the model estimates there could be a remaining gap in ICU capacity of more than 500 beds.
•Response Efforts:
In response, the Administration is aiming to find or build an additional 750 – 1,000 beds in field medical hospitals and other alternate care sites to reduce strain on hospitals as much as possible. Gov. Baker and Lt. Gov. Polito visited the first of these Field Medical Stations at the DCU Center yesterday.
The Administration has identified additional possible sites for Field Medical Stations including the Boston Convention & Exhibition Center, Joint Base Cape Cod, Springfield’s Mass Mutual Building and other smaller locations. The Administration has secured a contractor who can build out sites once a healthcare partner has been finalized.
The Command Center is also securing 1,000 beds in capacity for step-down care options in nursing facilities for stabilized COVID-19 positive patients who can be transferred out of the hospital to make room for those with higher medical need.
1 comment for “Gov. Baker says more ICU beds are needed; COVID death rate in Mass. is lower than other states”